St. Peter’s Urology provides the UroLift® System as a minimally invasion treatment option to treat Benign Prostatic Hyperplasia (BPH). BPH is a common condition that affects over 42 million men in the U.S.(1) and over 660 million aging men worldwide (2.3).
What is BPH?
BPH is a condition in which the prostate enlarges as men get older. Over 40% of men in their 50s and over 70% of men in their 60s have BPH (2). While BPH is a benign condition and unrelated to prostate cancer, it can greatly affect a man’s quality of life.
As the prostate enlarges, it presses on and blocks the urethra, causing bothersome urinary symptoms. If left untreated, BPH can lead to permanent bladder damage (4). Symptoms of BPH can cause loss of productivity, depression and decreased quality of life (7). BPH is the leading reason men visit a urologist (8).
Symptoms include (5,6):
- Frequent need to urinate both day and night
- Weak or slow urinary stream
- A sense that you cannot completely empty your bladder
- Difficulty or delay in starting urination
- Urgent feeling of needing to urinate
- A urinary stream that stops and starts
Treating BPH with Urolift
If you have been diagnosed with an enlarged prostate due to BPH, consult with your provider to determine which treatment is right for you. Along with watchful waiting, medications or surgery, minimally invasive treatment options include the UroLift® System.
Advantages of the UroLift System
- Safe and effective (2)
- Risk profile better than reported for surgical procedures such as TURP3
- Rapid symptom relief (4), better than reported for medications (5)
- Only leading BPH procedure shown not to cause new and lasting sexual dysfunction *(2,5,6)
- Covered by Medicare, national and commercial plans **
- Typically no catheter required after treatment (4,6)
Urolift uses small implants to open the prostate blockage and does not require heating or cutting tissue. The procedure is typically performed under local anesthesia in a doctor’s office and patients typically return home the same day without a catheter (6,8).
The UroLift System offers rapid symptom relief with a low risk profile (6). As the procedure does not destroy tissue, recovery on average is more rapid than for TURP patients. It is the only leading BPH procedure shown to provide symptom relief while also preserving sexual function* (8-11). Patients may experience short-term pelvic pain and light blood in the urine (6,7).
How Does The UroLift® System Work?
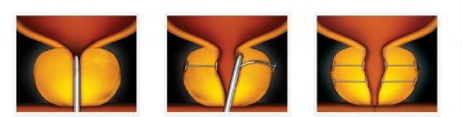
Step 1: The UroLift Delivery Device is placed through the obstructed urethra to access the enlarged prostate.
Step 2: Small UroLift Implants are permanently placed to lift and hold the enlarged prostate tissue out of the way and increase the opening of the urethra.
Step 3: The UroLift Delivery Device is removed, leaving an open urethra designed to provide symptom relief.
This treatment is indicated for the treatment of symptoms of an enlarged prostate up to 100 cc in men 45 years or older. As with any medical procedure, individual results may vary.
References
Read More
The information on this page was provided by UroLift®.
What is BHP section references:
- NeoTract US Market Model estimates for 2020, data on file.
- Berry, et al., Journal of Urology 1984
- US Census Bureau international database worldwide population estimates for 2020
- Tubaro, Drugs Aging 2003
- Rosenberg, Int J Clin Pract 2007
- Vuichoud, Can J Urol 2015
- Speakman, BJUI International 2014
- IMS Health NDTI Urology Specialty Profile Report 2013
Treating BHP with Urolift section references
*No instances of new, sustained erectile or ejaculatory dysfunction in the L.I.F.T. pivotal study
**When medical criteria are met
- AUA BPH Guidelines 2003. Updated 2010.
- Djavan, Urology 2004
- Chang DF, Campbell JR, J Cataract Refract Surg. 2005
- Duan et al, Pharmacoepidemiol Drug Saf. 2018
- Welk et al, JAMA Intern Med. 2017
- Roehrborn, J Urol 2013
- Roehrborn, Can J Urol 2017
- Shore Can J Urol 2014
- Tutrone, Can J Urol 2020
- Eure, et al., AUA 2020
- Sonksen, et al., Eur Urol 2015
For the full list of references and more information, click here.
